Lindsey Vonn’s ‘car crash’ injury explained: How long could her recovery take and will she ski again?
Two and a half weeks after her crash during the Olympic downhill race in Cortina d’Ampezzo, Lindsey Vonn has returned to the U.S. and is finally out of hospital.
In a video update posted on her Instagram page, she described the injury she suffered to her left leg as “by far the most extreme, painful and challenging I’ve faced in my life, times 100”.
Vonn is in a wheelchair and will be for a while as she also broke her right ankle in the crash. But what is her longer-term prognosis?
The Athletic spoke to orthopaedic trauma surgeon Ash Vasireddy, head of trauma at London’s King’s College Hospital’s Level-1 Major Trauma Centre and Cleveland Clinic London, and Caroline Bagley, a trauma and orthopaedic consultant at London’s Whittington Hospital.
How did Vonn suffer her injury and what happened to her leg?
Vonn arrived at the Winter Olympics with a full anterior cruciate ligament (ACL) rupture, bone bruising and meniscal damage in her left knee from a crash suffered at the final World Cup downhill race just before the Games. In Italy, she was competing with a specialised knee brace.
Following her crash at the Olympics, Vonn has stated that her prior ACL injury had nothing to do with fall in Cortina d’Ampezzo.
“Video footage from the fall shows her right arm hooking the gate, causing her to twist and fall rather than her knee giving way,” says Bagley. “Based on that mechanism, the fall appears to have been triggered by upper-body contact with the gate rather than knee instability or her knee brace.”
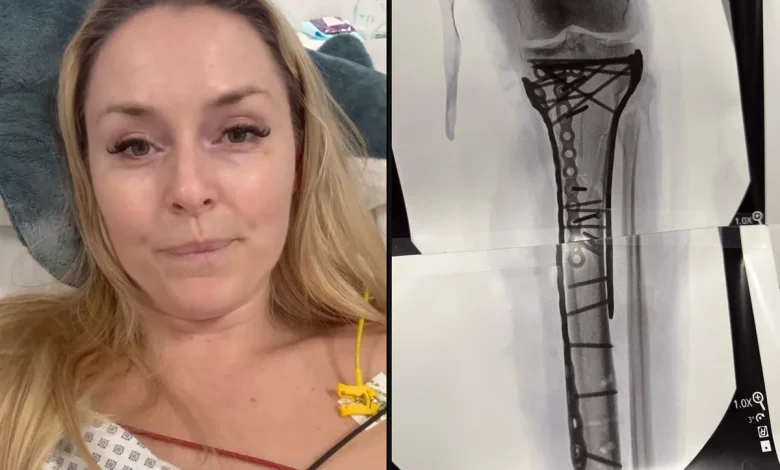
Vonn revealed that her injuries included a complex tibia fracture, a fracture of her fibula head and her tibial plateau: “Everything was in pieces,” she said.
“When Vonn crashed, she was careering down a mountain at close to 70 miles per hour,” says Bagley. “At that velocity, the forces involved are comparable to a serious road-traffic collision.”
Vonn with an image of her broken leg (lindseyvonn/Instagram)
The tibia is the shin bone and the fibula is the slimmer bone next to it. The tibial plateau is the upper surface of the tibia that forms part of the knee joint.
When a fracture is termed ‘complex’, it can mean a number of things, says Vasireddy. “In general, people use the term complex to mean a complicated fracture pattern — maybe the fracture is in multiple pieces. It can also mean fractures that involve different regions of the tibia.”
Whether the fracture is open or closed can also impact whether it is termed as complex. “The other thing is, whether there is associated injury,” says Vasireddy. “Is there injury to a blood vessel? Is there injury to a nerve? You can have any and all combinations of this.”
In Vonn’s case, the fracture extended into the knee joint, which Bagley says makes it even more serious: “When a break involves a joint surface, restoring perfect alignment becomes critical to long-term function,” she adds.
Vonn has also revealed that she suffered from compartment syndrome, a serious condition where excessive bleeding causes pressure to build dangerously in a closed compartment. Typically, this is an area in a limb containing muscles, blood vessels and nerves, usually enclosed by bone or other rigid structures.
“When you get swelling in that region, which typically in the case of trauma is from bleeding from a bone, that increases the pressure inside that space,” Vasireddy says. “That reduces the blood flow in the tiny vessels supplying the nerves and gives you this worsening pain that doesn’t respond to even the strongest painkillers. Those nerves are effectively having their blood supply strangled.”
Compartment syndrome is classed as an orthopaedic emergency. In the UK, the guidelines are that the patient should be inside an operating theatre within an hour of diagnosis.
Why was it so dangerous?
If compartment syndrome goes untreated, it becomes more and more and more painful, says Vasireddy. “The pressure becomes so high that it affects the blood flow in that whole region and effectively stops blood from reaching any of the tissues — nerves, muscles, anything — inside that space. Those structures effectively do not get a blood supply and wither away. Then the tissues start dying.”
When that happens, the tissues become a source of infection, because bacteria thrive in dead tissue. It can also significantly reduce function, with muscles ceasing to function and the leg becoming stiff. As Vonn said in her Instagram post, her surgeon, Dr Tom Hackett “saved (her leg) from being amputated”.
Vasireddy agrees that amputation is a recognised risk of compartment syndrome, particularly if the compartment syndrome evolved and there were complications like infection that weren’t able to be controlled despite multiple surgeries. It is, however, rare.
How is compartment syndrome treated?
Vonn explained that she had a fasciotomy, an emergency procedure where tissues are released to depressurise the region.
From the knee to the ankle, there are four compartments. A surgeon will typically do two incisions on either side of the leg (inner and outer) which go from near the knee down to near the ankle. “These are not small wounds,” explains Vasireddy. “You would cut the skin, cut the fat, and then you would cut the fascia which is this tight, almost clingfilm-like, tissue. You open it out and the muscles breathe a sigh of relief as the area is depressurised.”
If the surgeon finds any dead, devitalised tissues during the fasciotomy, they have to be removed to avoid them becoming infected.
Following the fasciotomy, the leg is left open at both sides for at least 24 hours, possibly a bit longer. But the bones cannot be left fractured and unstable during this time, so that’s when an external fixator would be used — as it was in Vonn’s case.
Vonn’s leg after one of her surgeries (lindseyvonn/Instagram)
An external fixator is a metal frame that “stabilises the bone from outside the body”, explains Bagley. “Pins are inserted through the skin into the bone above and below the fracture. These pins are connected to rods outside the leg, forming a rigid scaffold. If the fracture extends into the knee joint, like Vonn’s, pins may be placed in both the thigh bone and the shin bone to hold everything steady.
“The aim is to keep the fragments aligned, reduce pain and allow swelling to settle as well as protect damaged soft tissues.”
As for the wounds, which Vasireddy describes as being “like a long ellipse” in shape, they can be treated either with simple dressings made from gauze, wool and a bandage, or something more sophisticated such as a negative suction dressing, which draws fluid away from the wound.
When the patient is taken back to theatre, the muscle is checked to see whether it’s all healthy and there’s no damaged or devitalised tissue before the surgeon considers slowly starting to close them back up.
More often than not, the swelling does not shrink quite enough for it to all be stitched back together. “So you end up having orthopaedic surgeons and plastic surgeons working together,” says Vasireddy. One fixes the bone, while the other does skin grafting of the wounds, which adds to recovery time.
What about the fracture?
“Severe fractures like this are rarely fixed in a single operation,” says Bagley. “Swelling and soft tissue injury make immediate surgery risky. For that reason, treatment is usually staged. The first stage commonly involves an external fixator, then, once the swelling improves, surgeons can proceed to a further operation.”
There are three options for that next operation, depending on the nature of the fracture, where it is in the leg and what associated injuries there might be. Those options can be plates and screws, a titanium rod through the middle of the bone, which is locked in place with screws, and a circular frame which acts as a kind of scaffolding system for the leg, holding it in place with wires and pins.
In an update shared last week, Vonn described having a six-hour surgery that has left her with “a lot of plates and screws” in her leg. That metalwork may remain in place for life, although there are exceptions.
“The plates used in areas like the tibia can be quite prominent,” says Bagley, “and because the bone is close to the skin, patients may sometimes notice increased sensitivity in cold weather. A significant amount of metal can also interfere with things like CT or MRI scans.
“In Vonn’s case, it’s likely the hardware will be removed at some point, but only after complete healing. For now, that decision is probably far down the priority list.”
Lindsey Vonn is transported to hospital after her crash (Marco Bertorello/ AFP via Getty Images)
How will Vonn go about rehab now?
Vonn has said she is determined to return to the slopes, but, Bagley warns, “recovery from a complex tibial fracture is a long and demanding journey.”
Vonn will only be able to place weight on the leg once it has healed sufficiently and she has also said she will eventually need further surgery to fix her ACL rupture which will further extend her recovery timeline.
In the shorter term, Vasireddy says moving the joint as early as possible is a priority, to avoid it becoming too stiff. Gradually putting weight through the leg comes next, but generally only after around six weeks. This is important, says Vasireddy, not only for the muscle rehabilitation — to minimise the deconditioning of the muscles — but for patients to feel more ‘normal’.
In general, a tibial fracture can take around six to nine months to heal, depending the extent and nature of the injury to the bone and soft tissue.
After about three months, says Vasireddy, most people are beginning to walk and coming off their use of walking aids. That’s also around the time that an athlete would be looking to get back onto the training ground or, at the very least, into the gym. But those timelines can be prolonged by complications like compartment syndrome and blood vessel injuries.
In terms of rehab and recovery, Vasireddy says the starting point is always a focus on joint range of motion, followed by proprioception (joint balance) and then strengthening. “For most people, this is effectively a year out of significant sports,” he adds.
What’s the long-term prognosis — and will she ski again?
For Bagley, Vonn’s chances of a return are “difficult but not impossible, particularly for an athlete of her calibre. Elite athletes possess not only extraordinary physical conditioning but also exceptional mental resilience. Olympians’ bodies can at times surprise clinicians with the speed and extent of recovery, though even they are ultimately bound by the limits of biology.”
The potential long-term implications of an injury like this come from deconditioning. Vasireddy explains that the tolerance of our legs to be able to do the same amount of physical work is less. There can also be issues with chronic pain and sensitivity of the leg to cold temperatures. On top of that, the range of motion might be reduced from what it was before the injury and the power an individual is able to generate long-term would also be significantly at risk.
“The more issues you have, the weaker the leg will be in the long term, the less supple it will be,” says Vasireddy.
Does Vonn’s age and injury history impact her recovery?
“Age does influence recovery,” says Bagley, “but it’s only one factor. As people get older, their bone healing and rehab can take longer compared to younger athletes. However, someone like Vonn, who is exceptionally fit, disciplined, and has access to top-level medical care, would be expected to recover better than the average person of the same age.
“Being in good health, good nutrition and high-quality rehabilitation matter just as much as age itself.”
In Vasireddy’s view, the impact of previous injuries depends on where those injuries occurred in relation to her current problems, and whether those injuries had fully healed.
“If something’s been recently injured – say someone has damaged knee ligaments playing football and then gets on their motorbike two weeks later and has a nasty open fracture of the tibia or a tibial fracture with compartment syndrome – then yes, the rehab is a little bit concurrent and that can make it longer,” he says.
“Although, you would try and do the rehab simultaneously for everything, not sequentially.”





